Personalized Medication
Move from Populations to Personalized; Selecting drug therapy based on genomic testing to reduce ineffective treatment and waste as a result of trial-and-error prescribingSpecialty Drugs
Identifying the right patient with the right drug, acquired from a preferred pharmacy and administered in the right setting; Controlling costs while enhancing patient outcomesClaims Adjudication
RxAequitas™ is our own blockchain-based pharma ecosystem platform for secure transactions processing, transparency, and self-auditingFinancial Control
Control of your pharmacy benefit the way you want it; technology efficiency; customized plan design & formulary; greatly reduced costs; retain 100% of rebates and additional manufacturer incentivesNo Games
Fairness in service agreements with client-friendly language; Actual Acquisition Cost pricing disclosure; True 100% pass-through of all manufacturer incentives and pricing improvementsRx Pricing Transparity™
Transparency
Parity
Equity
"To make an omelet, you gotta break some eggs!"
Mutual Rx was created in response to prescription drug benefit plan sponsors' frustration with traditional pharmacy benefit managers (“PBMs”). Lack of trust, inconsistent pricing, along with little transparency, created the need for a better approach.

Headquartered in Southwest Florida, Mutual Rx’s seasoned pharmacy benefit executives have deep experience in the operational and management functions required to run a successful pharmacy benefit administration service. We bring this alternative to our client partners as a turn-key solution. Our model empowers drug benefit plan sponsors to provide PBM services to their members without the PBM!
Plan Sponsors We Serve
Unions
Employers
Public Sector
Health Systems
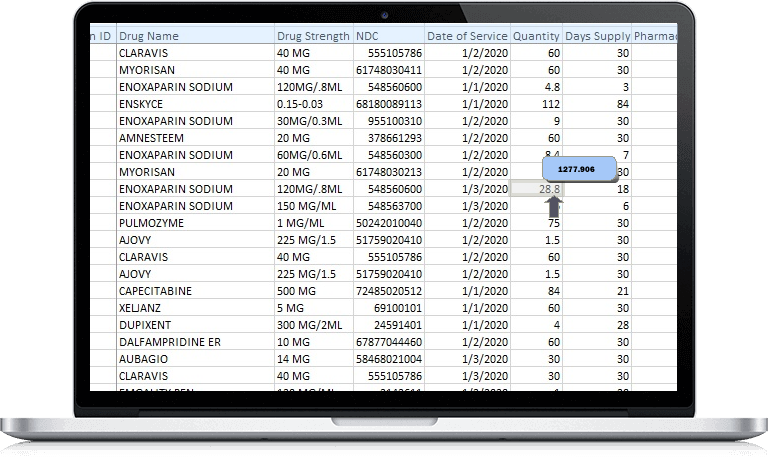
A Digital Health Company Dedicated to Improving Pharmacy Benefits
RxAequitas™ provides pricing transparency, self-completing administrative functions through the use of smart contracts, instant payment transfer to pharmacies, and is self-auditing by maintaining an immutable transaction record.
Learn MoreMutual Rx eliminates the traditional PBM "middleman" thereby reducing costs by 30% or more.

Our mission is to reduce prescription drug costs and improve patient outcomes through the use of pricing transparency, enhanced clinical insight and technology efficiencies.

Member Services
..Call center, member portal, Patient Care Advocate (PCA), clinical communications, mobile app, TelePharm
Clinical Programs
..Utilization review, step-therapy, auto prior-authorizations, medication therapy management, disease management, opioid care management, and other clinical support programs
Lowest Net Cost
..Customized formularies that don't chase rebates; eliminate low-value drugs; optimizing the use of generics and biosimilars
Performance
..No-risk guarantee. If we don't meet our PMPM cost-reduction forecast, we will make it good to the plan on a dollar-for-dollar basis!
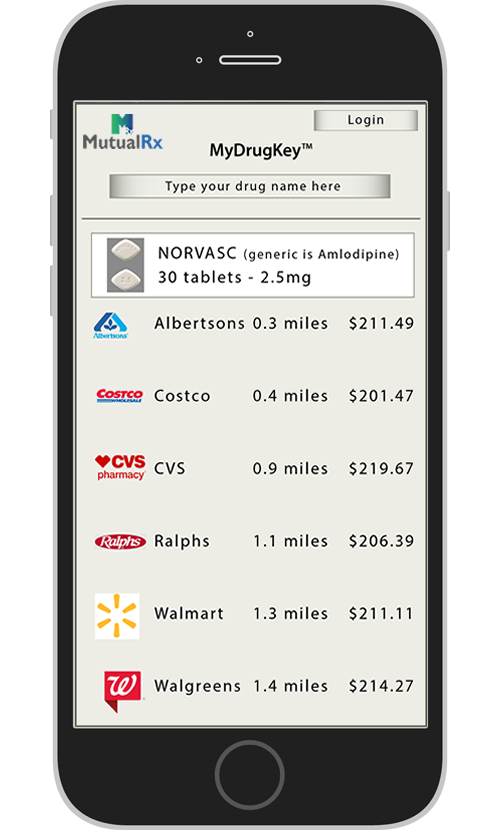
Lowest Net Cost Formulary
Personalized Member Services
Fiduciary Responsibility
The Mutual Rx Magic
How do we do it? Our national retail network contracts and rebate aggregation/GPO enables us to offer pricing and rebates similar to the biggest players. Because we don’t chase rebates, our drug mix creates huge cost savings by eliminating costly, but clinically valueless medications.
Additionally, we pursue distribution arrangements that best serve the needs of our clients and not tied to investment-driven profit forecasts. By operating on independence and greatly reduced margins, a client does not have to incur additional expense. Our operating efficiency provides clients with quality prescription drug coverage without sacrificing exceptional member service.
Contact Us
Our Leadership & Advisors

Roy Wilkinson
Founder & CEO
Greg Watanabe
COO
Michael Thompson
CAO
Mark Lucente
CTO
Andy Krause
CDO
Angela Wilson
CFO
Mei Tang, PharmD
VP-Clinical Programs
Hugh Easley, PharmD
Advisor
Rocco Calabrese
Advisor
Kay Plantes, PhD
Advisor
Gary Owens, MD
Advisor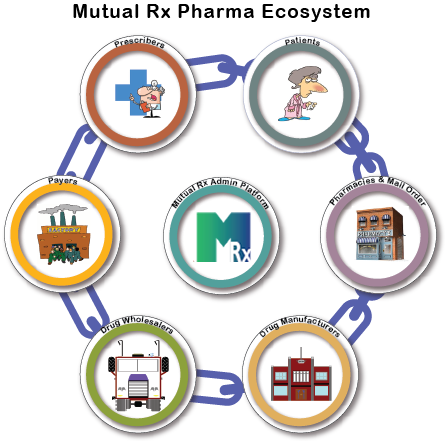
RxAequitas™ Platform
Our private cloud-based blockchain network is the pharmacy benefit platform of the future. Truthfulness, fairness, and equality in prescription drugs are the underlying foundation of RxAequitas™. Our model is built on blockchain technology and machine learning, which eliminates the need for a central controlling middleman. The network is designed as a decentralized distributed system, where designated stakeholders are a permissioned partner to complete transactions, without the dependency on a third-party entity for authentication, transparency and pricing trust. No longer will Plan Sponsors have to wonder whether the pricing information being shared by their traditional PBM is, in fact, an accurate representation of the market or their transactional applications. Transactions will be time-stamped, verified and adjudicated without delay and payments will be automatically made. There will be no need for human processing for approvals. There will also be no need to retroactively audit, because the system is self-completing and validates the entire claims process.
Contact Us



